Dr. Pankaj Gupta
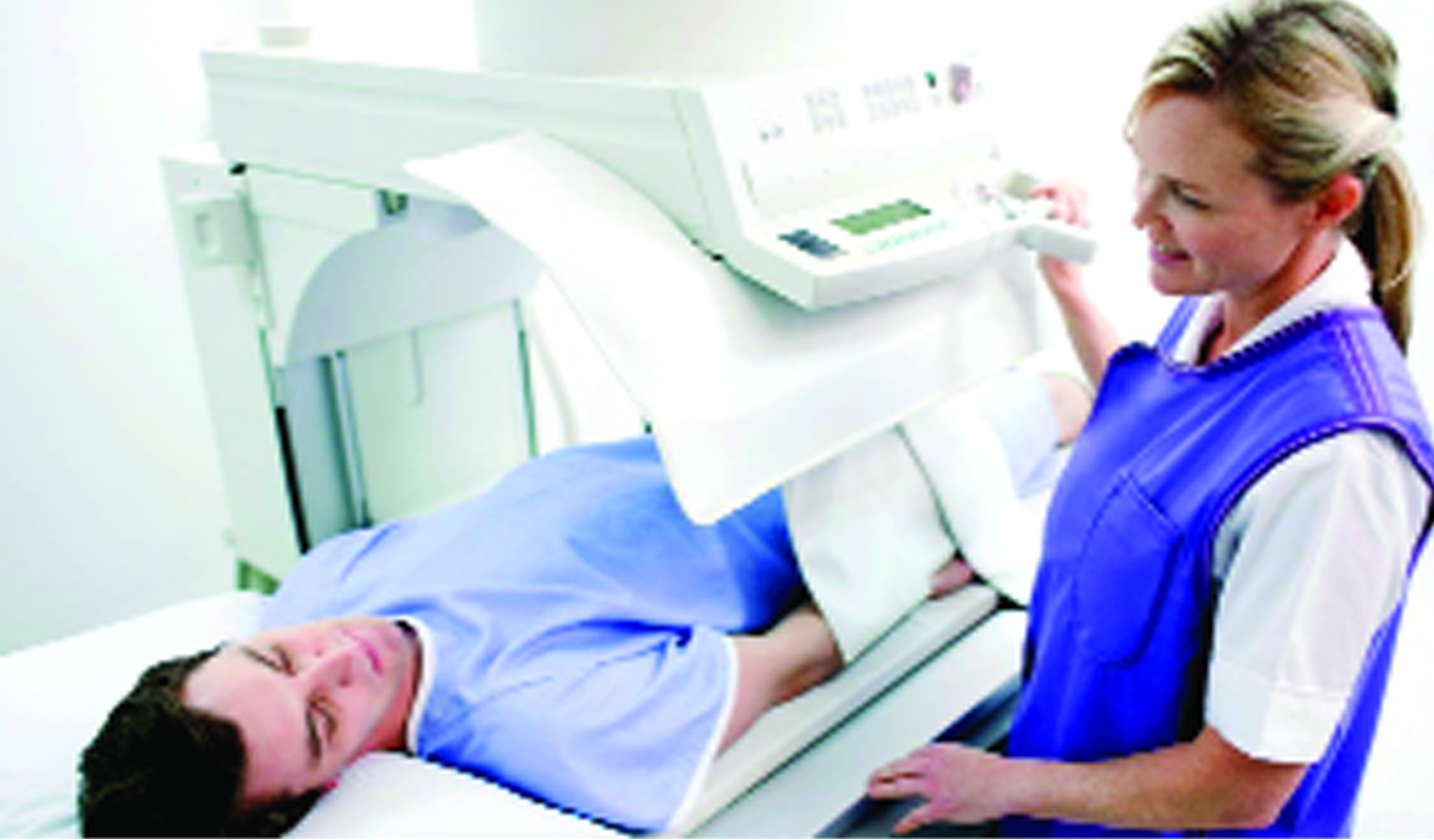
Interventional radiology (IR) is a sub specialty of radiology that deals with minimally invasive procedures (without a large ‘cut’ or incision on the body) that are performed under the guidance of imaging techniques like X-ray, ultrasound or computed tomography (CT) scan. Some of these procedures are done for diagnosis (venography, angiography, fine needle aspiration, biopsy), while others are done for treatment (for example, abscess or ‘pus’ drainage, endovascular embolization for treatment of internal bleeding). IR procedures are typically done with the help of needles and other tiny instruments (like small tubes called catheters, Figure) passed through the skin under constant visualisation with any of the imaging techniques described above. A radiologist with expertise in these procedures is called an interventional radiologist.
IR first came into existence in the mid 1970’s, when angioplasty and stent were first used in the lower limbs, to salvage patient with vascular disease. Since the late 1970s, IR has grown substantially and has become an integral part of patient care. In fact, IR has been the most significant medical development of modern times. Today many disease conditions which used to require surgery for either diagnosis or treatment are being dealt non-surgically with the help of IR. Few common examples are percutaneous biopsies (taking out piece of tissue) of liver, kidneys or masses (tumors) to establish the diagnosis of various diseases; drainage of abscesses (pus) in liver, kidney or other organs, drainage of fluid collections in chest or abdomen; varicose vein (dilated veins usually in the legs) ablation; endovascular management of bleeding in various organs e.g. brain. The extensive spectrum of procedures (both vascular and non-vascular) that IR caters to is however, beyond the scope of this article.
For the patients and their relatives, the minimally invasive IR procedures are nothing less than a boon. This is due to the fact that these procedures are associated with significantly lower risk to the patient, reduced pain (as large incision are not required), shorter period of hospital stays and faster recovery compared to conventional surgical procedures. Besides, most of the procedures can be done without general anaesthesia. This allows early return of the patient to the routine activities including work.
Unfortunately, in several part of the world there is lack of awareness about IR. This is due to the lack of infrastructure for training of post graduates in IR as well as lack of liaison between the interventional radiologist and the colleagues from other clinical specialities. This causes a great suffering to the patients as the disease conditions either remains undiagnosed or untreated or patient has to undergo extensive surgery with associated risks. Sometimes, patient may not be offered any treatment at all. In this regard, there is need for greater awareness among patients as well as doctors about the vast potential of IR so that this speciality is able to disseminate its benefits to our patients. In addition, There is a scope as well as need for greater coordination among the physicians (including interventional radiologist) for promoting IR and making it a routinely practiced speciality for the good of the society.
USG guided aspiration of liver abscess
Some of the hardwares used by interventional radiologist
(The author is a M.D. Radiodiagnosis (AIIMS, New Delhi).
Trending Now
E-Paper