Dr Mandeep Kaur
Oral ulcer is the loss or of delicate tissue that lines the inside of the mouth. The most common cause is injury (such as accidentally biting the inside of your cheek). Because of variety of presenting features and causative factors, identification of oral ulcers may be challenging for a dentist or a general clinician to reach a conclusive diagnosis.
Malignant Ulcers
Most patients with oral ulcers will have symptoms for more than two weeks, reflecting the early sign of malignancy. Most common malignancy in oral cavity is oral squamous cell carcinoma which appears as a non-healing and non-tender crater-like ulcer with the indurated rolled border. The common sites are ventral and lateral borders of the tongue, the floor of the mouth and lower lip.
Ulcers Due to Microbial Agents
Ulcers due to microbial agents (virus, bacterial and fungal) typically appear as vesiculobullous lesions that initially appear as intact blisters which eventually rupture leading to ulcerations. HSV type-1, herpes zoster, EBV, HIV infection has clinical presentations as ulcers. The bacterial infection presenting with oral ulcers are necrotising ulcerative gingivitis, noma, TB and syphilis. Fungal infection infrequently results in oral ulceration.
Ulcers due to Hormonal Imbalance
The imbalances in the hormones are present in numerous diseases related to endocrine system of the human body as pregnancy and puberty. It is expressed as increased salivary estrogen level provoke local changes such as increased exfoliation of the oral epithelium causing ulcerations in oral cavity among females during the normal menstrual cycle and pregnancy.
Ulcers due to Systemic Disorders
Systemic disorders such as chancre, ANUG, oral cancer, leukaemia, traumatic abscess, cyclic neutropenia results in oral ulcers. Most of the time, the oral site can act as the first indication of blood born disease before other signs and symptoms appear. Pernicious and iron deficiency anemia may present with superficial and small ulcers.
Ulcers due to Inflammatory Bowel Diseases
The most frequent inflammatory bowel disease (IBD) includes ulcerative colitis and Crohn’s disease. Lesions of the oral cavity may be apparent and last for months to a year. Most common oral manifestation of IBD during its active phase is characterised as deep linear ulcers, having rolled edges which involve the buccal vestibules.
Ulcers due to Immune-Mediated Disorders
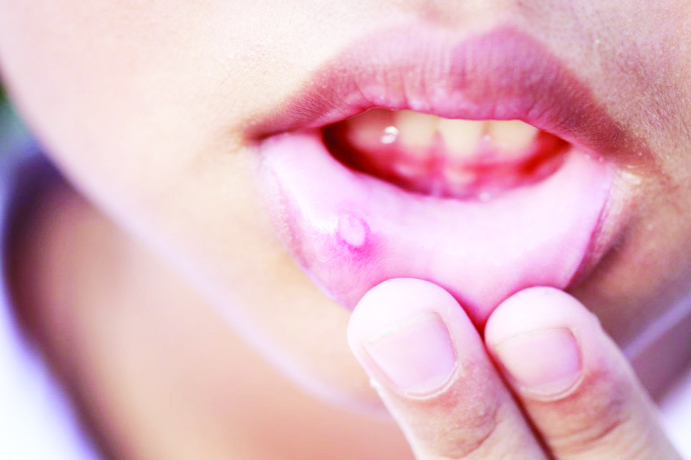
One of the most common inflammatory lesions of the oral cavity is known as “Recurrent Aphthous Stomatitis”. Clinically, it is described by oral ulceration recurrent episodes in an otherwise healthy individual. It can be categorised as minor aphthous, major aphthous and herpetiform. Ulcers appear as a rounded, tender mucosal surface covering with fibrin slough surrounded by an erythematous border.
Vesiculobullous Lesions of the Oral Cavity
Vesiculobullous immune-mediated diseases like mucous membrane pemphigoid pemphigus vulgaris, erosive lichen planus can present with chronic and multiple oral ulcerations of oral mucosa and discomfort.
Traumatic Ulcers/ Iatrogenic/Idiopathic Ulcers
Injuries due to trauma affecting the oral cavity may result in the surface ulcerations. Sublingual ulcerations are seen in newborns and infants occurs in Riga-Fede disease. The traumatic ulceration in children occurs due to thermal or electrical factors especially at corner of lips whereas in adults the traumatic ulceration is the result of mechanical injuries like malformed or fractured teeth; ill-fitting dentures; overheated foods and radiation injuries.
Treatment
* Avoid spicy and sour foods until the ulcers heal.
* Drink plenty of fluids.
* Keep your mouth clean.
* Apply antiseptic gel to the ulcers.
* Regularly rinse your mouth out with warm, slightly salted water, keeping the rinse in your mouth for up to 4 minutes at a time.
* Use an alcohol-free mouthwash twice daily.
* If required in severe cases, immunosuppressant medication may be prescribed by your oral health professional.
Oral ulceration diagnosis needs a thorough history taking and clinical examination. The fact cannot be denied that oral presentation may be a sign of some underlying systemic disease. Any ulcer that lasts longer than two weeks should be examined his to pathologically. This helps the dental clinicians to create a stepwise method to rule out doubtful conditions to reach a definite diagnosis.
(The author is Assistant Professor Dept of Oral Pathology & Microbiology Indira Gandhi Govt Dental College, Jammu)
Trending Now
E-Paper